Valv = RR x (V T-V D) = RR x V T – RR x V DĬonsequently, for a steady minute ventilation, when the respiratory rate or the dead space are increased, alveolar ventilation is reduced. Secondly, the dead space which is the “wasted part of the breath” intervenes more frequently when respiratory rate increases.Īlveolar ventilation (Valv) is the efficient part of the minute ventilation for gas exchange. The weight of dead space increases in proportion of tidal volume decrease. Firstly, with low tidal volumes, the V D/V T increases as tidal volume decreases if V D remains constant. The use of small tidal volumes (V T) and high respiratory rates (RR) has several consequences in terms of alveolar ventilation and dead space. Impact of protective ventilation settings With protective ventilation and reduced overdistention, the alveolar dead space may be reduced.Īll the different parts of the dead space are also taken into account in the VentilO application. The alveolar dead space is not counted, consequently, the total dead space is underestimated. The next figures are built, based on the calculations of the dead space detailed in the study. Most efficient HME have usually a volume above 50 ml (up to 90 ml), catheter mount may have a volume of 20-60 ml, many connectors may be used in patients (CO 2 cuvette, closed suction and other adaptors for inhalation therapies) and may represent an important additional dead space. Instrumental dead space may be very high (above 100 ml) when counting HME, catheter mount, connectors and endotracheal tube. 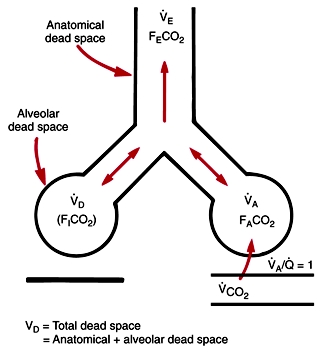
Part of the instrumental dead space is not easily reduced: the endotracheal tube (ETT) may be changed for a tracheostomy tube to reduce the dead space by 10-12 ml, or ETT may be cut but the gain is very limited (2-4 ml). Part of the instrumental dead space may be easily limited by reducing the number of useless connections and by using a heated humidifier instead of a heat and moisture exchanger (HME) for gas humidification. Dead space may be divided into instrumental dead space and physiological dead space (including airway and alveolar dead space). 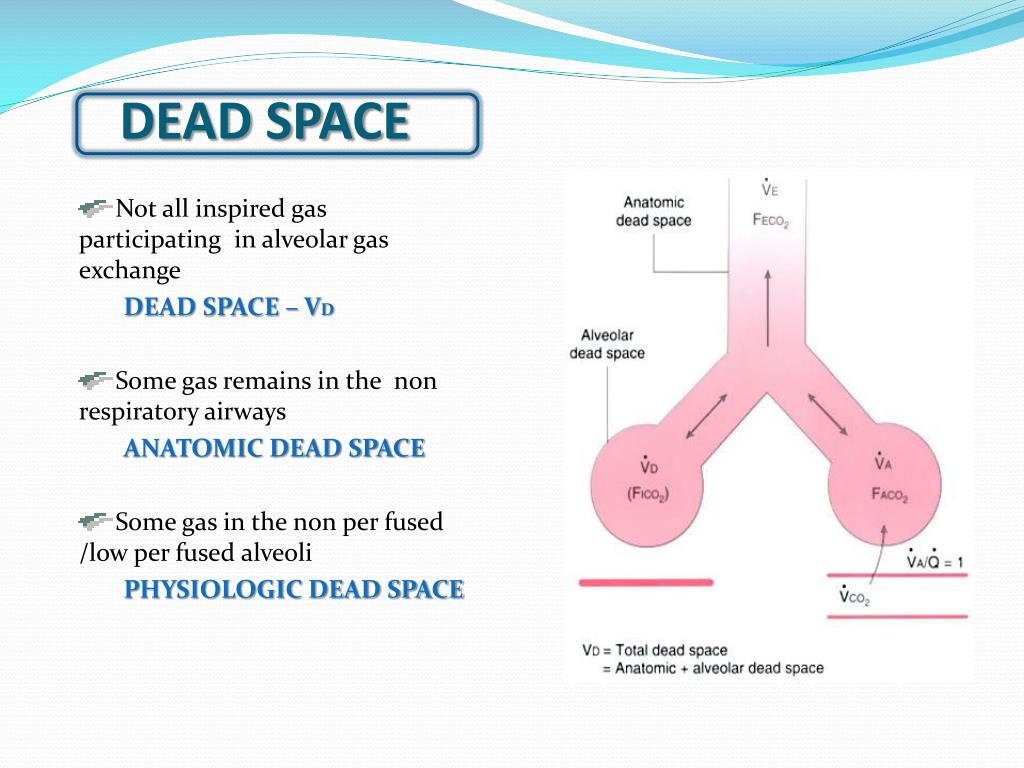
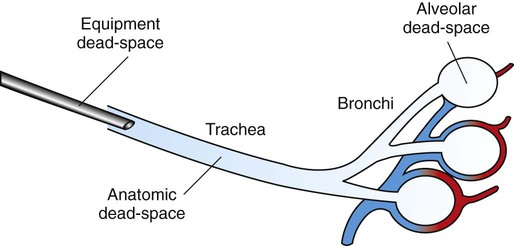
Using a heated humidifier instead of a filter is a very efficient way to reduce this dead space.įigure 1: The figure represents the different portions of the dead space. From the lungs to the patient, the alveolar dead space may be reduced by limiting overdistention the dead space of the airways is difficult to modify and is mildly increased by PEEP and bronchodilation the instrumental dead space is the easiest to modify, may account for almost half of the total dead space and include the humidification filter at the Y-piece, the CO 2 sensor, the connections, catheter mount, flex tube, etc. Surprisingly, however, in virtually all studies evaluating respiratory mechanics in ARDS or in COVID-19 patients, the instrumental dead space is not provided nor mentioned, even when V D/V T is evaluated! The different parts of the dead space in mechanically ventilated are as follows. Many studies showed its large impact on the work of breathing during assisted ventilation and on alveolar ventilation during controlled ventilation. Often, the instrumental dead space is overlooked during mechanical ventilation. What is the dead space during invasive mechanical ventilation? Consequently with low tidal volumes and high respiratory rates the weight of the dead space (also referred to as VD/VT) is automatically increased. The alveolar ventilation is defined as the respiratory rate times (tidal volume – dead space volume). Based on the recently published paper “Impact of Respiratory Rate and Dead Space in the Current Era of Lung Protective Mechanical Ventilation”, we will discuss here briefly the different part of the dead space and how it can be reduced, as well as the relations with respiratory rate, tidal volume and alveolar ventilation (part 2).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
